A Belgian Hospital Cut off Ajima Ogbole’s Cervix. Then They Paralysed Her Sister-In-Law Susan (VIDEO)
When a surgery went wrong at Belgian hospital AZ Sint-Jan, Ajima Ogbole’s desire to birth a child was thwarted, prompting her sister-in-law to act as a surrogate. But Susan Ogbole, the surrogate, became crippled after giving birth at the same hospital. With one unable to ever carry a pregnancy and the other potentially unable to ever walk again, the Nigerians are tossed around in Belgium, the hospital unwilling to take responsibility for the traumatic, life-defining alterations to their lives.
Hours after the surgery to remove fibroid from Ajima Ogbole’s uterus was completed at the Obstetrics and Gynecology unit of AZ Sint-Jan Hospital in Bruges, Belgium, she woke up believing that the obstacle she was told could prevent her from having a child had been surmounted. But she was wrong; her cervix was amputated during the surgery. Problem compounded.
In early 2017, she had been diagnosed with uterine fibroid by doctors in Belgium. According to Ajima’s medical report, translated from Dutch and seen by FIJ, a Magnetic Resonance Imaging (MRI) scan confirmed the presence of multiple subserosal fibroids – growths around the uterus. It is “without signs of complications”, the report stated.
Before Dr. Van de Vijver performed the surgery to extract the fibroid in November 2017, Ajima was prescribed medications to reduce the size of the fibroids. The surgery was successful; about 13 fibroids were removed.
THE TRAUMATIC POST-RECOVERY JOURNEY
During a post-surgery checkup in January 2018, an MRI scan was done, but the cervix, a tiny passageway linking the uterus to the vagina, was not found.
“I checked and I think it is blocked. We’ll need to put an Intrauterine Device (IUD) to keep the hole open,” Ajima said, recalling what the Belgian doctor told her.
But when she returned to the hospital few weeks later, expecting to have an IUD insertion, Dr. Van de Vijver, without prior notification, performed laparoscopy, a diagnostic medical procedure to examine internal organs such as the uterus and the cervix. She was deceived; her right as a patient to not receive treatment she did not give informed consent to was breached!
“They put me under anaesthesia and when I woke up, I had four holes on my tummy, which was a laparoscopy and I didn’t know at the time,” she told FIJ. “I remember asking my husband if IUDs were usually sewn on the skin and from inside of the uterus. For me, it was strange.”
THE FRUITLESS SEARCH FOR HER CERVIX
She did not know the complexity of her situation when the doctor informed her that her cervix could not be found. Medical report described her cervix as “sharply altered”. Ajima was subsequently referred to a professor of Gynaecology at UZ Leuven, an academic hospital, who could re-create her cervix.
At UZ Leuven, before agreeing to help her, the professor said he would take her off the medication Dr. Van de Vijver had placed her on to cease menstruation. The professor thought it was strange that the doctor kept her on the medication after the surgery, Ajima said.
About five weeks later, she had her period in severe pain and blood did not flow out of her vagina — it flowed backward. The professor told her that the retrograde menstruation puts her at risk of endometriosis (which causes pelvic pain) and slim chances of cancer if her body continues to absorb the ‘bad blood’. She was given two options: continue taking medications to hold off her period or remove her uterus.
The professor then examined her reproductive system with a medical device hoping to find a bubble, which would mean that there was a connection between the vagina and the uterus. But he did not find. The complexity of the situation became clear when Ajima and her Belgian husband talked to the professor.
“What the doctor asked me to do can never be done,” she recalled in tears. “A cervix has never been successfully re-created medically.”
Even if one was re-created, there were risks: when pregnancy becomes heavy, there could be a tear. Or there could be other complications, including infections. He warned her to not allow anyone cut her open, as such efforts would be “trial and error”.
‘YOU CAN’T GET PREGNANT AGAIN’

“In fact, he said I could’t get pregnant naturally or artificially because the connection between my cervix and my vagina was gone and that my best option was surrogacy,” she said.
Ajima returned home that day, switched off her phones for three weeks and wept.
“I never believed that this was what my life had turned into. I knew I wanted kids more than I wanted to get married. The possibility of becoming a mother had been taken away from me,” she lamented.
Together with her husband, she travelled to Nigeria to be with family. While in the country, she sought opinions from two experts in Abuja and Plateau State. Both told her to forget about getting pregnant.
MENSTRUAL HAPPINESS
After six months of waiting, another professor of Gynaecology who specialises in reconstructive surgery at the University of Ghent performed a laparotomy – used to diagnose or treat abdominal health conditions – on her. But it was unsuccessful. Ajima had been told the chance of success was slim.
“By chance of success, he (professor) didn’t mean to get pregnant, he meant to successfully re-create the hole that connects to the vagina first so that I can at least have my period and then try to see if they can help me get pregnant. So, when I was told that it was not successful, I could not cry; I was just numb.”
Two weeks later, she decided to take up the professor’s offer to try another reconstructive surgery. After the procedure, she had her period. “I never knew I would be so happy to see my period,” she said.
Her period flowed for three months and then it gradually stopped and began spotting (A period is spotting when there is hormonal fluctuation and bleeding is lighter than a normal flow.).
FOUR SURGERIES IN TWO YEARS
The four surgeries she had within two years still cause a lot of discomfort to her entire being.
She said: “At a point, I recovered physically but internally, I still feel pains. I am not in a good place mentally, psychological and emotionally. I can’t fully perform my matrimonial duties as I am always pained, bruised or with blood.”
Ajima’s career as an architect, fashion designer and entrepreneur have also suffered. Her plan was to shuttle between Belgium and Nigeria because of her business, but surgeries and constant visits to hospitals have made that impossible.
FIGHTING THE BELGIAN HEALTH SYSTEM TO HAVE A BABY

In Belgium, having a child through a surrogate is not easy. Although commercial surrogacy is not illegal, it is in a legal grey zone area; there is no law that protects parties involved if issues such as filiation and nationality occur.
Also, hospitals regulate themselves, consequently possessing the freedom to arbitrarily decide whom to take on as surrogacy candidates. The best option for Ajima and her husband was the United States, but it was too expensive.
A glint of hope came when Susan, the wife of Ajima’s younger brother and a mother of two children aged three and five who was moving to Belgium to study at the Free University of Brussels, agreed to be a surrogate for the couple. Susan’s husband consented.
But their perfect plan was set back when hospitals in Belgium, including the one where the cervix error was made, would not accept Susan as a surrogate. Ajima said that they were worried for the safety of the child whose nationality at birth would also be Nigerian.
They had to travel to Nigeria for the IVF treatment, including embryo creation and implanting in Susan. It was successful, so they returned to Belgium. Everything went smoothly except that during the first trimester, she was ill many times.
FROM CHILDBIRTH TO PARALYSIS
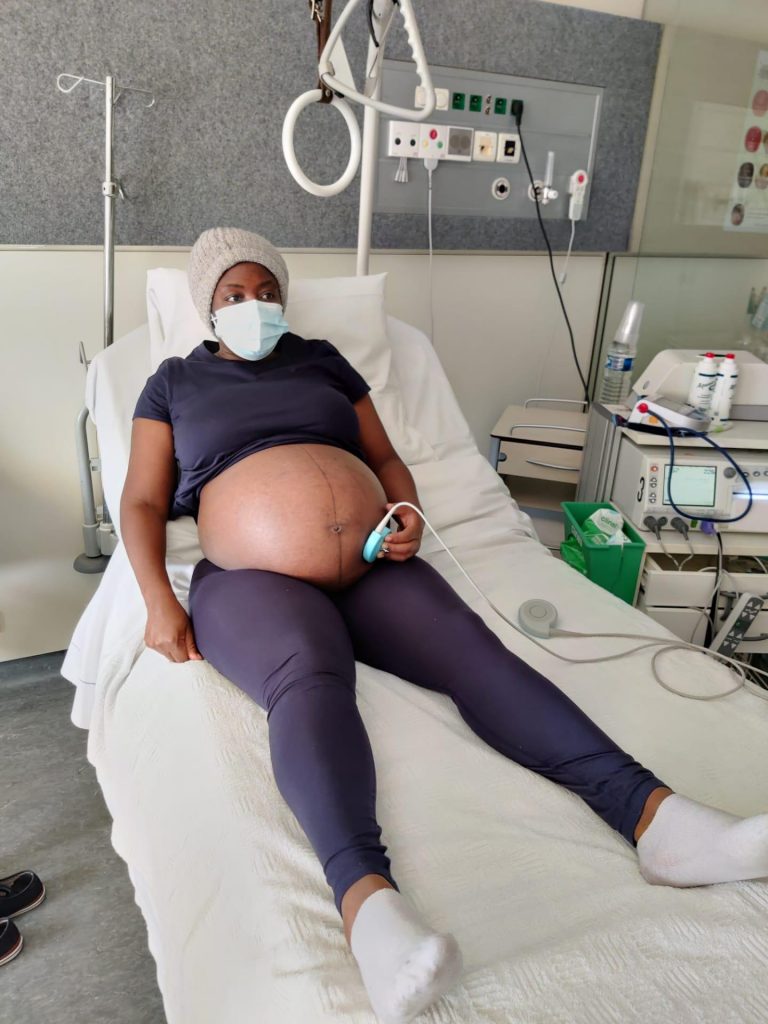
After birthing a healthy baby at AZ Sint-Jan Hospital on the morning of October 15, 2020, Susan lost control of both legs. The family was traumatised and abandoned by – the same hospital where Ajima’s cervix was mistakenly amputated.
Susan made two requests during one of her visits to the doctor before the baby was born: a caesarean delivery and a general anaesthesia – a medication that would make her unconscious. She had always been scared of an epidural.
The Belgian doctors agreed to a caesarean section, but advised her to choose an epidural because they wanted the baby to be awake when she was born or she would be taken to the neonatal intensive care unit. Susan agreed reluctantly.
Her medical report showed that she was given a combined spinal epidural anaesthesia — local anaesthetic is injected near a spinal cord and nerve roots to block pain from an entire region of the body such as the belly, the hips and the pelvis.
Ajima said that her mother, who is a nurse and midwife, discouraged Susan from taking epidural, as there could be problems if improperly done. One of the problems is temporary or permanent nerve damage, which may be caused by direct damage to the spinal cord, infection in the area near the spinal cord or accidentally injecting the wrong medicine in the epidural catheter.
Susan cried and writhed in pains during the epidural procedure, as Dr. Van Laere Freya, an anaesthesiologist who was supervised by Dr. Geertrui Delrue, prepared her for surgery. Ajima told FIJ that Susan was given the anaesthesia by a resident in anaesthesiology.
“When this resident was giving her, the ombudsperson in the hospital said that the supervisor told her she was there but was not putting on gloves. She just stood aside. It is like giving a resident a heart surgery to do and you are standing there and watching; any little thing can ruin somebody’s life,” she said.
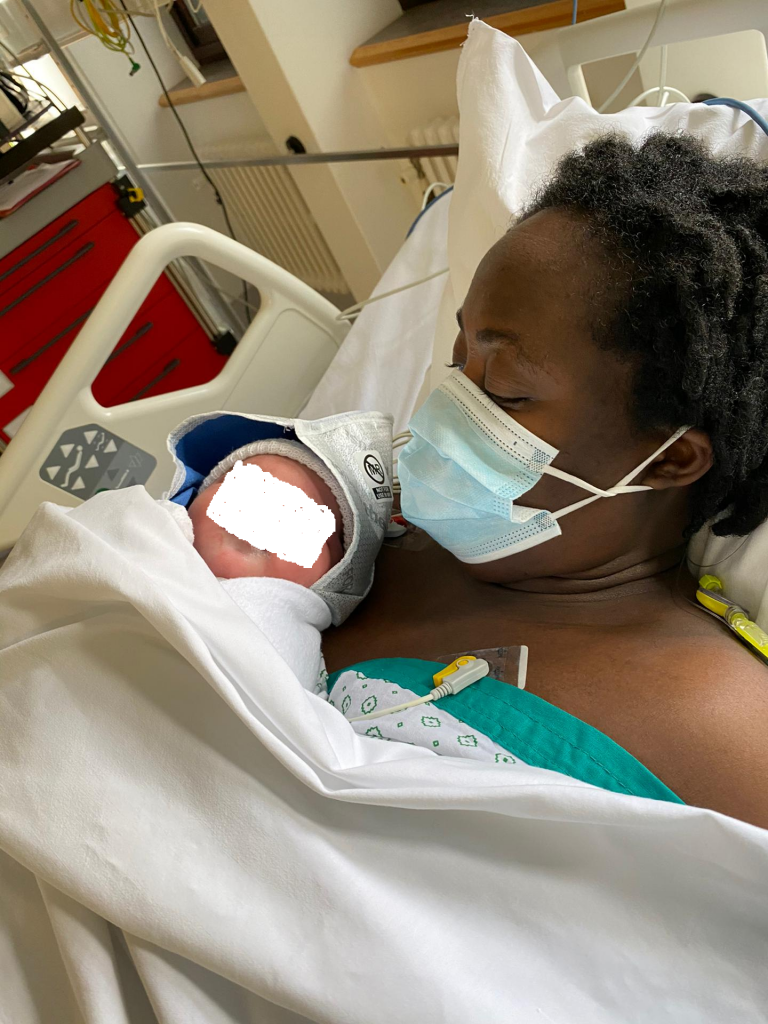
When her epidural was taken out after she gave birth, Susan could not stand without being supported.
“I can’t feel my legs,” Ajima remembered Susan crying out. The anaesthesiologists and neurologists found nothing. By the third day, Susan could not feel anything from her waist down. She had become paralysed.
‘AFRICAN BACTERIA’ — THE ‘CONSPIRACY’ TO COVER-UP A MEDICAL ERROR
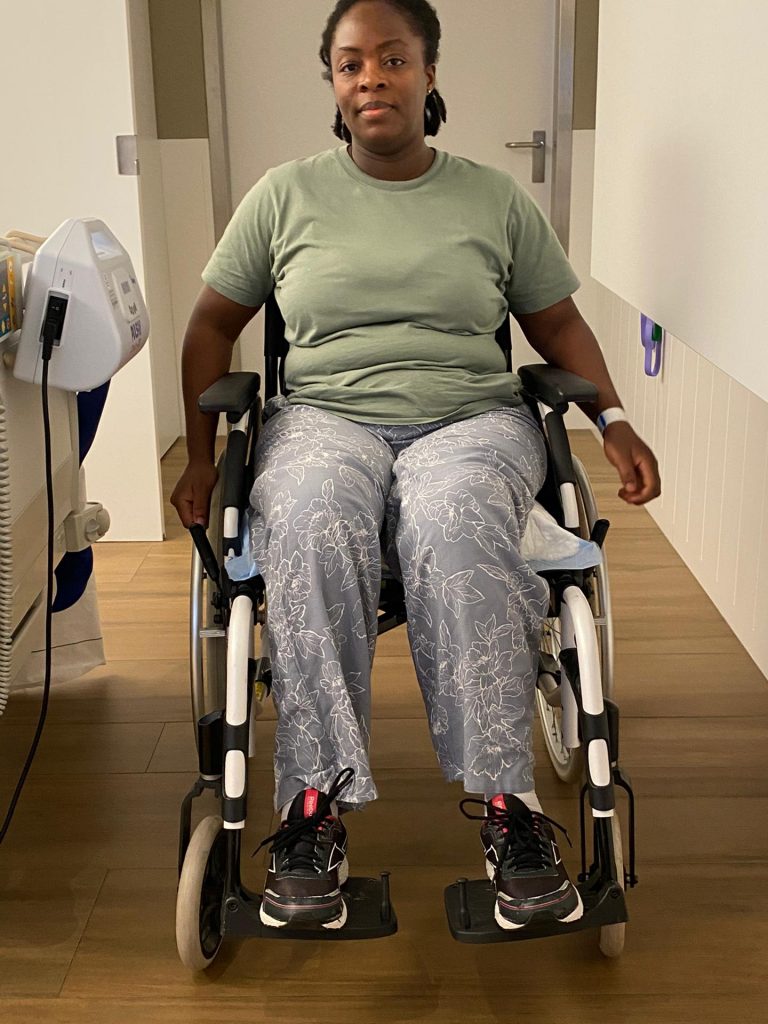
Susan’s medical report, seen by the FIJ, described the pregnancy as uncomplicated but medical staff described her situation after giving birth as a complication. Family members are accusing the hospital of covering up the medical error that resulted to Susan’s paralysis.
“They claimed it was an African bacterial infection because they don’t have that particular bacteria in Europe,” Ajima said. “It didn’t make sense because Susan had been in Belgium for about a year. To cover what they did, they pumped her with antibiotics but she is still unable to walk. They could not even provide the name of the African bacteria.”
She said a US-based anaesthesiologist told her that if it was a bacterium, it shows negligence because it suggests that either the equipment or her back, where the epidural went through, was not properly sterilised.
Suspicious of the Belgium hospital, the family sought second opinion from a retired professor of anaesthesiology.
“If it was a bacterium infection, Susan would have gone into coma, would have had high fever and would have been hallucinating,” Ajima recalled the retired professor writing in an email.
Despite disagreeing with the hospital’s diagnosis that Susan became paralysed because of a bacterium infection, the professor was silent on the question about whether a nerve was hit. In fact, he told the family that he would not grant a request to give an opinion if the issue goes to the court.
Susan’s family disagrees with some details in her obstetric report by AZ Sint-Jan Hospital. The claim that Susan had postpartum fever was denied. “The doctors used claims of fever as a pretext to pump antibacterial into her system in order to cover up what they did wrong,” Ajima claimed.
GRAM STAIN TEST REVEALS THERE WAS NO BACTERIAL INFECTION
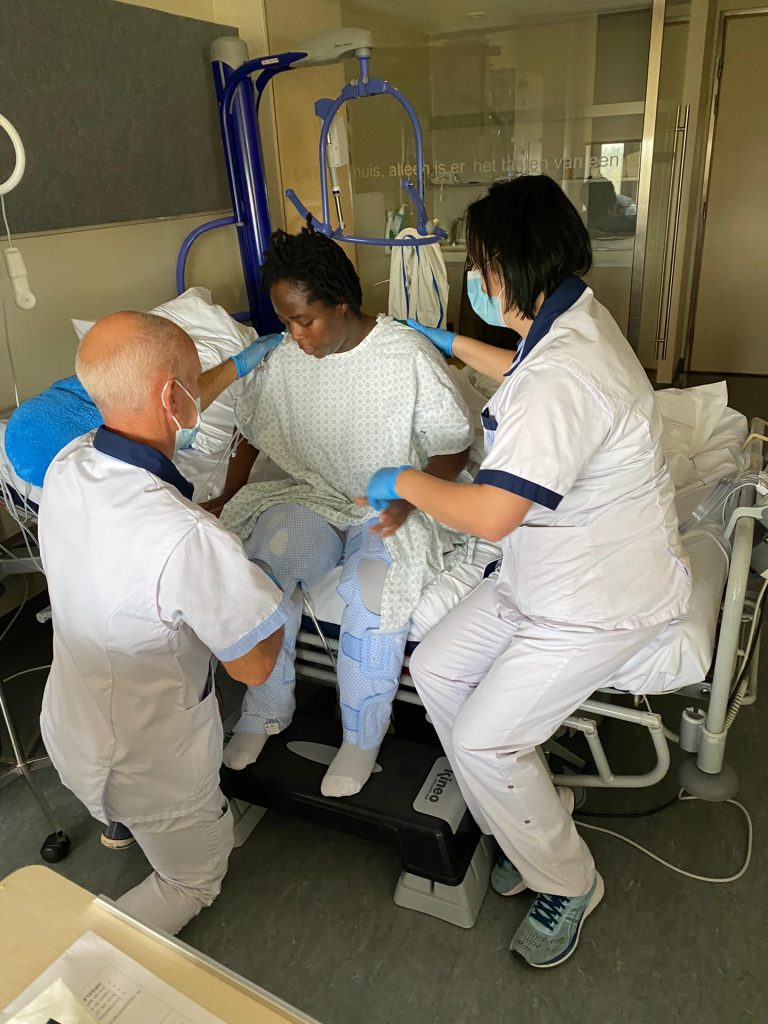
The report revealed that she was given two antibacterial medication and one antiviral medication.
“But even if it’s a bacterium, as she’s been pumped with antibiotics for more than two weeks, Susan should be on her feet now, four months after,” she said.
Also, a gram stain test done on the fluid from her spinal cord, post-birth, showed that no bacteria was present.
The anaesthesiologists who operated on Susan stopped checking on her after the family raised concerns to the hospital, FIJ was told. They claimed that because they had been accused of racism and causing Susan’s paralysis, attending to her would be an admission of guilt, Ajima said. Dr. Van de Vijver, the gynaecologist who made Ajima’s medical error and operated on Susan, later distanced himself from the family. Susan’s family believe that he was instructed to stop seeing them.
It was the closest hospital to us,” Ajima said when asked why they returned to the same hospital after what happened to her. “And we did not believe that a mistake would happen again because the doctor who made the mistake asked to be given another chance.”
Ajima said that some staff of AZ Sint-Jan said they were sure that the medical team that operated on her sister-in-law made an error and was doing everything to cover it.
Before Susan’s transfer to the hospital at the University of Ghent, AZ Sint-Jan ran some tests and reported on the evening of December 18, 2020 that she had Covid-19. She was moved to the coronavirus floor. Susan’s family felt it was plot to infect her with the disease because two previous tests done within 10 days came back negative. After pressure from her family, she was transferred to Ghent.
PARALYSED, THEN DENIED FAMILY SUPPORT BY BELGIAN AUTHORITIES

Since Susan’s childbirth process went wrong, Ajima, who still experiences aches from the four surgeries she has had in less than two years, had been left with caring for the baby and providing support for her sister-in-law.
Her mother-in-law would have come to help; two children who had not seen their mother for years would have visited but the Belgian government denied them visas. Ajima said the reason was concerns that they might not leave Belgium, as they had applied for family reunion.
However, Susan’s husband was issued a one-month visa instead of the one year multiple-entry visa he applied for to enable him visit his wife as many times as possible. In a mail, the country’s ministry of interior told the family that the one-month visa issued was a “favour”. A letter from the hospital stating that Susan would need support from her family was brushed aside.
The Kingdom of Belgium’s Foreign Affairs, through its Advisor, Barbaix Kristiaan, citing privacy reasons, did not tell FIJ why the Ogboles were denied visas. The Belgian Embassy in Nigeria gave the same reason for not answering questions from FIJ.
Both the Nigerians in Diaspora Commission (NiDCOM) and the Nigerian Embassy in Belgium did not respond to multiple requests for comments.
SURGEON ASKS BEDRIDDEN SUSAN TO ‘COME TO MY OFFICE’
The hospital did not give the Ogboles an official explanation for the fatal results of the treatment of two members of a family. Istead, it directed them to talk to its insurance firm.
Ethias, the hospital’s insurer, assigned Dr. Goegebuer, an orthopaedic surgeon, to evaluate Ajima’s gynaecology case and Susan’s suspected anaesthesiology and neurology situation.
Dr. Goegebuer asked Ajima whether she had a cervix before the surgery, if she was in the country legally and what she did for a living in Belgium. The initial conclusion that the amputation of her cervix was a complication was later reviewed to medical error after Ajima contended it. However, negotiation for compensation continues to drag on, as both parties could not agree on a fee.
In a letter to Susan, seen by this newspaper, Dr. Goegebuer instructed her to come to his office to “hear your story and to determine the physical damage”. But her lawyer, in response, said that the doctor did not review Susan’s file — because if he did, he would have known that she was immobile.
“Since December, when he said he would go to the hospital to meet her, he has not gone. Our lawyer wrote him three times, but he did not respond,” Ajima said.
WHY AN EPIDURAL CAN GO WRONG
When FIJ contacted Meysmans Saartje of Ethias, he said the firm does not comment on medical treatments. “This is forbidden in respect to privacy,” he explained.
However, a medical expert who did not want to be named told FIJ that the removal of subserosal fibroid is not difficult.
“So, for the cervix to be cut during the surgery, that worries me,” he said. “However, it depends on the location of the fibroid. It is possible that it happened while the doctor was removing the fibroids close to the cervix.”
He noted that Dr. Van de Vijver went against the ‘universal law’ of the profession when he performed a surgical procedure on Ajima without informing her of details such as what would be done and why.
“You are not supposed to cry and complain of pains during an epidural. It means the needle went amiss,” the expert said about Susan’s reaction to the procedure. “The skin is usually anaesthetised so that as the epidural is done, there won’t be pain.”
He agreed that something was not right with the epidural anaesthesia she was given, but noted that the tiny epidural needle, even if it hits a nerve, “will be transiently traumatised and the nerve will recover”.
“It is not supposed to paralyse a person for a long time,” he added.
The medical expert explained that surgeries, even those that are seemingly not risky, could go wrong at any time and that allegations of negligence would require in-depth investigations. But no investigation will occur with the hospital and its insurer ignoring the family.
“In a medical process, you may do harm while trying to do good; it is not intentional. When issues like this happen, we can only hope that people will speak the truth and live up to the scrutiny of their good conscience if they have anything like that,” he concluded.
NOT THE FIRST TIME
There are many cases of life-altering medical errors in Belgium. Most times, victims do not get justice because medical workers are treated like ‘demigods’ who cannot be questioned.
The country’s health system is structured such that medical workers are shielded from being held responsible for errors that occur while performing their jobs. Left unprotected, medical error victims bear the brunt of this system.
The system gives medical workers the impression that even when they do tawdry jobs, they will get away with it. And they do get away.
FIJ got reports of two other people who are victims of medical errors in Belgium. In one case, a woman who was given an injection became paralysed; she subsequently died. In the other, a woman’s legs were mistakenly amputated at a hospital in Bruges. The woman is currently seeking other victims of medical error to fight alongside her because on her own, she cannot afford the legal costs, with Belgium’s health system positioned to protect medical personnel from being held accountable for on-the-job errors.
AJIMA OGBOLE’S DEMANDS
Ajima wants Susan, who can’t travel, to be reunited with her family. She also wants the hospital to apologise and take full responsibility for the fatal results of the treatments she and her sister-in-law had. And she wants the Belgian health system to be overhauled to protect patients.
“If it happened to two family members in the same hospital, then we are hundred percent positive that it’s not just us,” she said.
“It’s not just about us, but people coming after us as well as the people before us who didn’t get the justice they deserved.”
Watch Video below:





